Vitamins for joint pain and stiffness are nutrients that support inflammation control, cartilage maintenance, muscle function, and bone health. The strongest evidence exists for correcting deficiencies, especially with vitamin D and omega-3 fatty acids. Some supplements may help certain people, but none reliably “fix” arthritis or reverse joint damage.
Joint supplements are one of the most overmarketed areas in health.
After reading the actual studies, the pattern becomes obvious:
- A few nutrients genuinely matter,
- A few are probably overhyped, and
- Many people are trying to solve mechanical joint problems with capsules alone.
Those are different problems.
- Vitamin D helps most when deficiency exists, not as a universal joint cure.
- Omega-3s have the strongest support for inflammatory joint pain.
- Glucosamine and collagen show mixed results despite aggressive marketing.
- Knee pain often has mechanical causes that supplements alone cannot fix.
- Women over 40 may benefit from better vitamin D, protein, and strength training support.
- Diet quality, sleep, movement, and weight management often matter more than expensive supplement stacks.
What causes joint pain and stiffness in the first place?
Joint pain and stiffness usually come from inflammation, cartilage wear, injury, autoimmune activity, or age-related joint changes. The cause matters because vitamins do not work equally well for every type of pain.
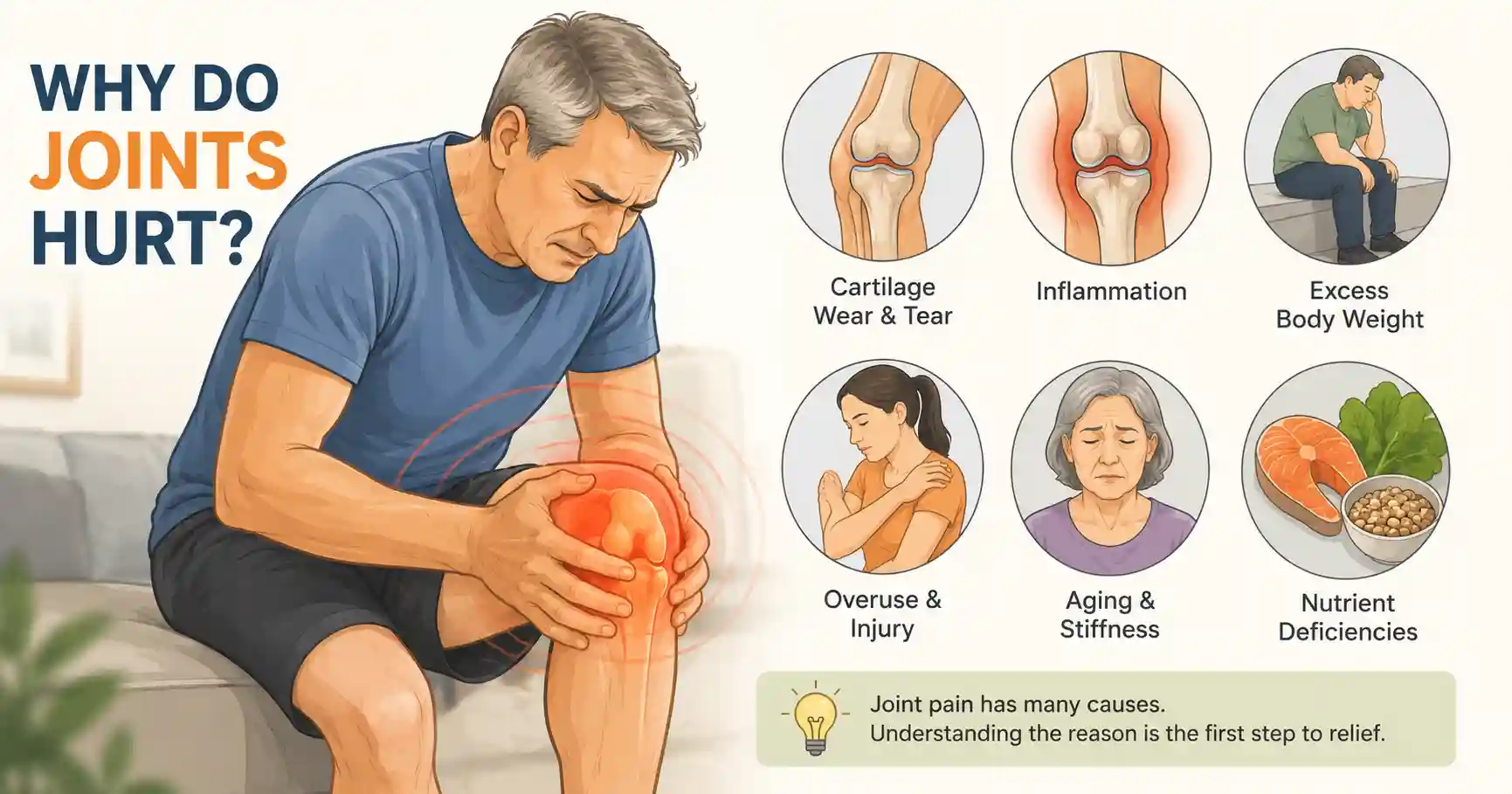
A stiff knee after sitting for an hour is not the same as swollen finger joints from rheumatoid arthritis. Yet most supplement articles treat them like identical problems.
The most common causes include:
- Osteoarthritis — cartilage breakdown over time
- Inflammatory arthritis — immune-driven inflammation
- Vitamin deficiencies — especially vitamin D
- Muscle weakness around joints — often overlooked
- Excess body weight — increases knee joint pressure
- Overuse injuries — tendons and connective tissue irritation
This matters because supplements mainly affect:
- inflammation pathways
- nutrient deficiencies
- connective tissue support
They do not rebuild severely damaged joints.
A surprising thing in the research: many adults with chronic joint pain also have low vitamin D levels. But low vitamin D may sometimes be a marker of poor overall health and inactivity, not necessarily the direct cause of the pain itself.
Which vitamins for joint pain and stiffness have the strongest evidence?
Vitamin D, omega-3 fatty acids, and magnesium currently have the strongest evidence for supporting joint comfort and reducing inflammation in some people. Evidence for glucosamine and collagen is mixed.

Here is the reality most supplement ads avoid.
| Nutrient | Evidence Strength | Best Use Case | What It Does NOT Do |
|---|---|---|---|
| Vitamin D | Moderate | Deficiency-related pain and stiffness | Does not rebuild cartilage |
| Omega-3s | Moderate | Inflammatory joint pain | Does not reverse arthritis |
| Magnesium | Emerging | Muscle tightness and stiffness | Not a direct arthritis cure |
| Vitamin C | Limited but useful | Collagen formation support | Cannot repair damaged joints alone |
| Glucosamine | Mixed | Mild osteoarthritis in some people | Does not work consistently |
| Collagen peptides | Mixed | Mild stiffness support | Evidence remains inconsistent |
Vitamin D
Vitamin D affects:
- immune regulation
- muscle function
- bone metabolism
Low levels are strongly associated with musculoskeletal pain. According to the NIH Office of Dietary Supplements, deficiency remains common in older adults, especially people with limited sun exposure.
A 2016 study published in JAMA found vitamin D supplementation did not significantly reduce knee pain progression in many adults with osteoarthritis who were not severely deficient. That detail gets skipped constantly in wellness content.
The nuance matters:
- Deficient people may improve
- Non-deficient people may notice little difference
That is a huge distinction.
Omega-3 Fatty Acids
Omega-3s from fish oil may help reduce inflammatory signaling. Evidence is strongest in rheumatoid arthritis rather than simple age-related stiffness.
Some people expect fish oil to work like pain medication. It does not. Improvements are usually modest and gradual.
Magnesium
Magnesium is interesting because joint pain and muscle pain often overlap.
Low magnesium may contribute to:
- muscle tension
- cramps
- poor sleep
- stiffness
This is why searches like “vitamins for joint pain and muscle pain” are becoming more common.
More Articles For Joint Pain
- Vitamins for Joint Pain and Stiffness: What Actually Helps?
- Joint Genesis Reviews 2026: Honest Look at Complaints & Results
- Can Gluten Cause Joint Pain? Causes & Symptoms Explained
- Big Toe Joint Pain Walking, Bending & Standing: Causes & Treatment
- Home Remedies for Gout Flare Up: What Works and What Fails
- Joint Genesis Reviews 2026: What Complaints Real Users Have!
Does vitamin D help joint pain if you are not deficient?
Vitamin D helps most when a deficiency exists. Research becomes much less convincing in people who already have normal vitamin D levels.

This is where online advice gets sloppy.
Those are not the same statement.
According to current research as of 2026:
- Severe deficiency correction matters
- Routine mega-dosing does not consistently improve arthritis outcomes
- Benefits vary widely by person
People with a higher risk of deficiency include:
- adults over 50
- people with obesity
- indoor workers
- people with darker skin tones
- postmenopausal women
The frustrating part is that vitamin D became a kind of “universal fix” online. The data simply does not support that level of confidence.
What is the difference between glucosamine, collagen, and vitamins?
Vitamins support body processes, while glucosamine and collagen are structural compounds linked to cartilage and connective tissue. They work differently and have different evidence quality.
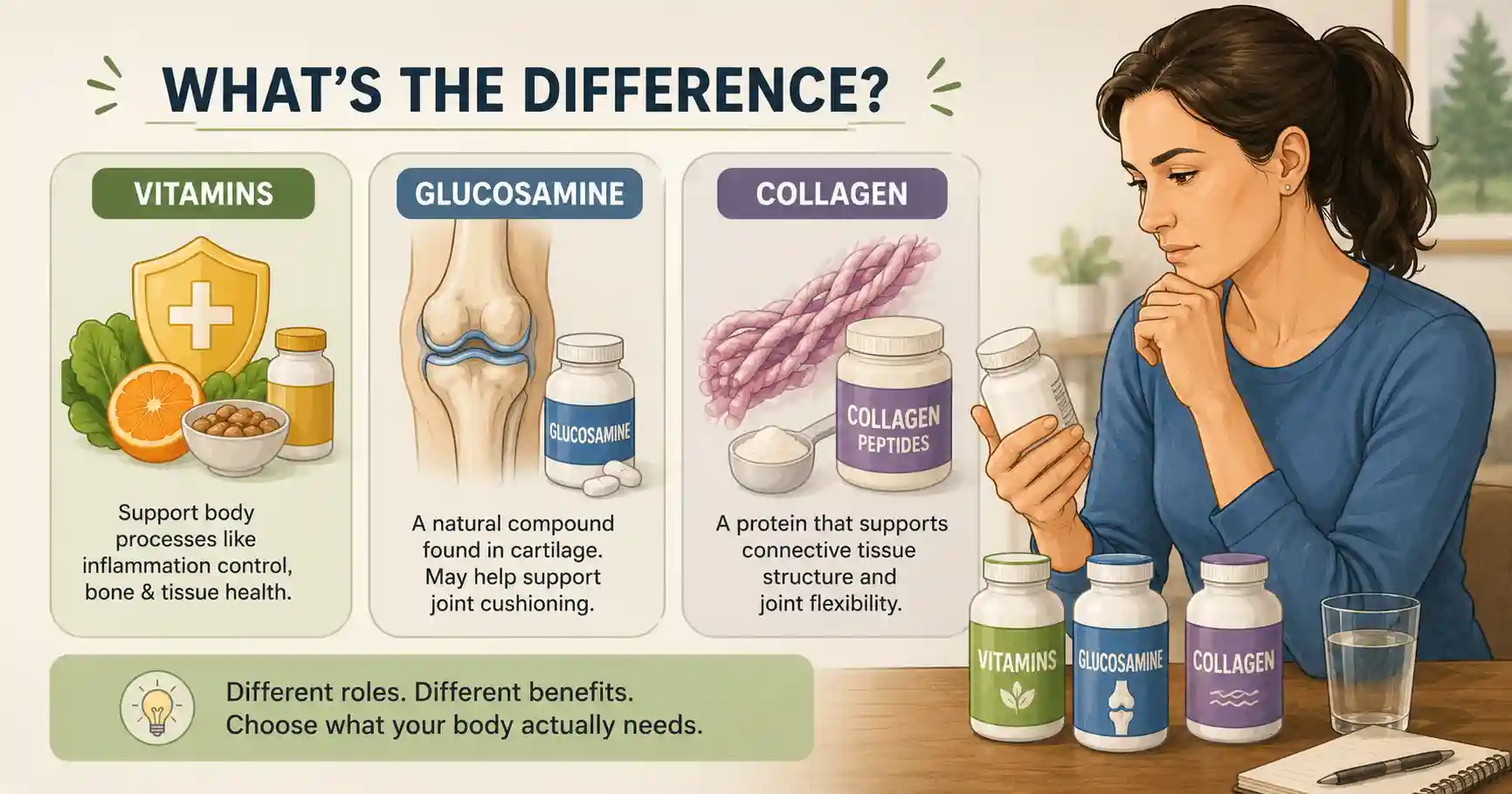
This gets confused constantly.
Vitamins
Vitamins mainly support:
- inflammation regulation
- bone metabolism
- tissue repair
- immune balance
Examples:
- Vitamin D
- Vitamin C
- Vitamin E
Glucosamine
Glucosamine is a naturally occurring compound found in cartilage.
Research results are inconsistent:
- Some knee osteoarthritis studies show modest relief
- Others show almost no difference from a placebo
Formulation matters more than many people realize. Prescription-grade glucosamine sulfate performed better in some European studies than cheaper over-the-counter blends.
Collagen
Collagen supplements aim to support connective tissue structure.
Evidence remains mixed:
- Some small studies show mild improvement
- Others show limited clinical benefit
The marketing around collagen got ahead of the science years ago.
That does not mean collagen is useless. It means the evidence is not nearly as dramatic as social media claims.
Which vitamins may help with knee pain, hand stiffness, and inflammation?
Different joint problems respond differently to nutritional support. Knee pain, inflammatory swelling, and hand stiffness are not identical conditions.
For knee pain
The most relevant nutrients are:
- Vitamin D
- Omega-3s
- Magnesium
- Glucosamine (mixed evidence)
But knee pain often has a mechanical component:
- excess body weight
- weak quadriceps
- cartilage wear
No supplement fixes poor joint mechanics.
For hand stiffness
Hand stiffness is more associated with:
- inflammatory arthritis
- autoimmune activity
- repetitive use
Omega-3s may help with inflammatory symptoms more than cartilage-related pain.
For inflammation
Research around anti-inflammatory support focuses mostly on:
- omega-3 fatty acids
- Mediterranean-style eating patterns
- maintaining a healthy body weight
Ironically, diet quality often matters more than isolated vitamin supplements.
That part gets ignored because “eat better and move more” is much harder to market than capsules.
Are vitamins for joint pain different for women over 40?
Women over 40 experience hormonal and bone-related changes that may influence joint stiffness, inflammation, and pain sensitivity. Vitamin D, calcium, protein intake, and resistance training become more important after menopause.
This is a major gap in most ranking articles.
Estrogen decline affects:
- bone density
- inflammation signaling
- connective tissue health
Many women notice:
- morning stiffness
- knee discomfort
- hand pain
- reduced recovery
Vitamin D deficiency also becomes more common during and after menopause.
But here is the important clarification: Joint pain in women is not automatically a “vitamin deficiency issue.”
Sometimes the bigger factors are:
- sleep disruption
- lower muscle mass
- inactivity
- weight gain
- inflammatory conditions
Supplements can support these issues. They rarely solve them alone.
Why do some people feel no improvement from joint supplements?
Many people see little improvement because the underlying problem is structural, mechanical, or unrelated to nutrient deficiency.
This is probably the most important section in the article.
Reasons supplements may fail include:
- The pain source is not nutritional
- torn cartilage
- advanced arthritis
- tendon injuries
- Expectations are unrealistic
- people expect painkiller-level results
- The evidence for the supplement is weak
- especially with heavily marketed blends
- Body weight is the bigger issue
- Knee joints absorb massive forces during walking
- Movement patterns matter more
- Weak hips and legs increase joint stress
One consistent pattern from real-world reports, including Reddit discussions, is that people who combine:
- strength training
- weight management
- anti-inflammatory eating
- sleep improvement
…tend to report better outcomes than people relying on supplements alone.
Not flashy. Just repeatedly true.
What foods naturally contain vitamins for joint pain relief?
Whole foods provide vitamins, minerals, antioxidants, and anti-inflammatory compounds together, which may support joints more effectively than isolated supplements alone.
| Food | Main Nutrients | Potential Benefit |
|---|---|---|
| Fatty fish | Omega-3s, Vitamin D | Inflammation support |
| Yogurt | Calcium, protein | Bone and muscle support |
| Citrus fruits | Vitamin C | Collagen support |
| Nuts and seeds | Magnesium, healthy fats | Inflammation balance |
| Leafy greens | Vitamin K, antioxidants | Bone support |
| Beans | Magnesium, protein | Muscle and tissue support |
A pattern seen in arthritis research is that dietary patterns matter more than “superfoods.” Mediterranean-style eating repeatedly shows better inflammation outcomes than ultra-processed diets.
FAQs
What vitamins for joint pain and stiffness work best?
Vitamin D, omega-3 fatty acids, and magnesium currently have the strongest evidence for helping some people with joint pain and stiffness. Benefits are usually more noticeable in people with nutrient deficiencies or inflammatory conditions. Evidence for glucosamine and collagen remains inconsistent across studies.
Do vitamins help with arthritis pain?
Some vitamins may help support inflammation control and muscle function, which can indirectly improve arthritis symptoms. They do not reverse arthritis or rebuild damaged joints. Lifestyle factors such as body weight, exercise, sleep, and diet quality usually have a larger long-term effect.
What vitamin deficiency causes joint pain?
Vitamin D deficiency is the most commonly linked deficiency associated with joint and musculoskeletal pain. Low magnesium levels may also contribute to muscle tightness and stiffness. Blood testing is often needed because symptoms alone are not reliable for identifying deficiencies.
Are glucosamine supplements worth taking for knee pain?
Research on glucosamine is mixed. Some people with mild osteoarthritis report modest relief, while others notice no difference at all. Formulation quality appears to matter, and benefits tend to be smaller than supplement advertising suggests.
Can vitamins help joint pain in the hands and feet?
They may help if inflammation, deficiency, or connective tissue support issues are contributing factors. Hand and foot pain caused by autoimmune arthritis, nerve issues, or structural degeneration often requires broader treatment approaches beyond supplements alone.
Our End Note
Joint supplements are not useless. But the internet tends to treat them like they work with the consistency of prescription medication. They do not.
For most people dealing with vitamins for joint pain and stiffness, the best approach is usually boring and unsexy:
- correct real deficiencies
- improve diet quality
- maintain muscle strength
- reduce excess joint stress
- Use supplements selectively instead of blindly stacking them
That approach is harder to market. It also lines up much better with the actual evidence.




Recent Posts