The best thing for sciatic nerve pain is a combination of gentle movement, targeted stretching, and anti-inflammatory medication — started early and kept consistent. Sciatica happens when the sciatic nerve is compressed or irritated, typically by a herniated disc or a tight piriformis muscle.
Most people recover within 6 to 12 weeks using conservative home treatment, without surgery or injections.
Key Takeaways
- Movement beats rest for sciatic pain — gentle activity keeps discs nourished and prevents nerve sensitivity from increasing.
- NSAIDs target the real issue — ibuprofen and naproxen reduce inflammation, unlike acetaminophen which only dulls pain.
- Sleep position directly affects nerve pressure — side sleeping with a pillow or back sleeping with knee support reduces compression.
- Morning pain has a physical cause — spinal discs rehydrate overnight, making early movement essential to avoid flare-ups.
- Pregnancy-related sciatica needs a different approach — avoid NSAIDs; focus on physical therapy and pelvic support.
- Targeted stretches work better than generic ones — figure-4 and knee-to-shoulder stretches directly relieve piriformis pressure.
What Is the Sciatic Nerve — and Why Does It Hurt So Much?
The sciatic nerve is the longest in the human body. It starts in the lower back, passes through the pelvis and buttocks, and runs down the back of each leg. When something presses on it, pain can shoot from the lower back all the way to the foot.
Here’s what most people miss: sciatica isn’t one condition with one cause. There are two main sources of nerve irritation, and the distinction changes how you treat it.
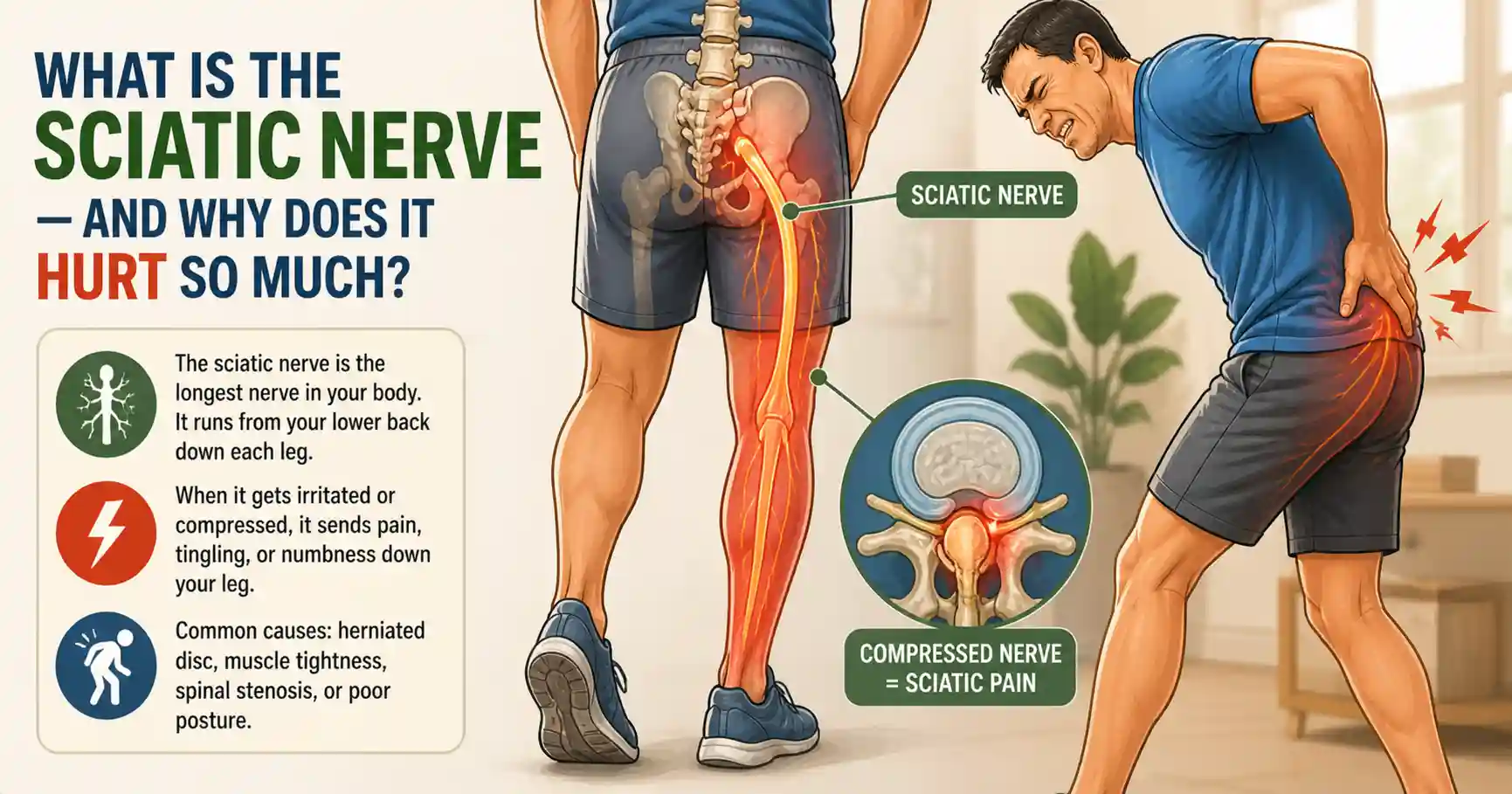
- Disc compression — a herniated or bulging disc pressing on a lumbar nerve root. Pain typically worsens when sitting or bending forward.
- Piriformis syndrome — a deep buttock muscle that spasms and traps the sciatic nerve nearby. Pain worsens after prolonged sitting and responds quickly to hip-focused stretching.
Getting these two confused is why a lot of treatment advice doesn’t work for everyone. The exercises that help disc compression can sometimes aggravate piriformis syndrome, and vice versa.
According to StatPearls (Davis et al., 2024), the lifetime incidence of sciatica ranges from 10 to 40 percent. It’s one of the most common causes of leg pain seen in medical care.
Quick Takeaway: Sciatica is a nerve issue with different root causes, and the cause you have determines which treatment actually works.
What Is the Best Thing for Sciatic Nerve Pain?
Movement is the single most effective treatment for most cases. Not aggressive exercise. Just consistent, gentle activity.
Most people reach for rest. That’s the wrong instinct.

Here’s the reason it backfires: the intervertebral discs in the spine have no direct blood supply. They absorb nutrients through a process called load cycling — the compression and decompression that happens naturally when you walk or change positions.
Lie still for days, and this exchange slows down. Inflammation builds up around the nerve root. Pain signals intensify.
A Cochrane review comparing bed rest to staying active for acute sciatica found that advised activity was at least as effective as rest, and in some measures, meaningfully better. The research on this has been consistent for decades.
What this means in practice
- Walking: yes, even short 10–15 minute sessions
- Lying still all day: no
- Avoiding every movement that feels uncomfortable: no
- Pushing through sharp nerve pain down the leg: also no
There is a real difference between discomfort from moving and nerve pain from compression. The first is manageable. The second is a signal to stop and adjust position.
Quick Takeaway: Staying gently active beats bed rest. This isn’t a close call in the research.
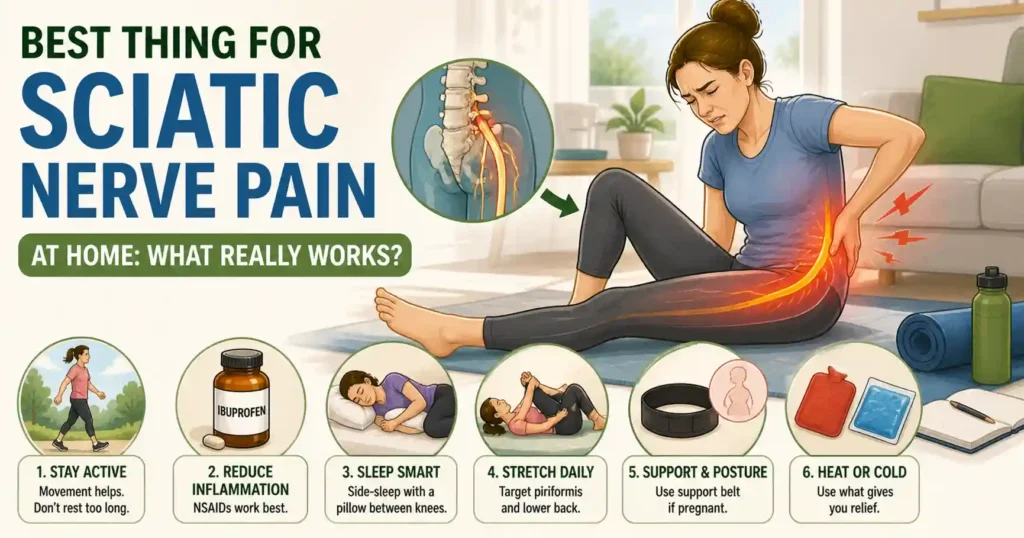
Best Home Remedies for Sciatic Nerve Pain
Home treatment works for most people. The problem isn’t the remedies — it’s the order.
1. Ice first
Apply an ice pack wrapped in cloth to the lower back or buttocks. Fifteen to twenty minutes, up to three times a day, during the first 48–72 hours. Cold reduces prostaglandin activity, limits swelling, and lowers the pain signal coming off the nerve.
2. Heat after 72 hours
Switch to heat once the acute inflammatory phase settles. A heating pad encourages blood flow, relaxes the piriformis and hamstrings, and reduces the muscle guarding that tightens defensively around an irritated nerve.
- What most people get wrong: Most people reach for heat immediately because it feels good. Heat applied during active inflammation increases localized swelling around the nerve root. It can extend a flare for days. The sequence matters more than most content lets on.
3. Walking
Ten to fifteen minutes of slow, flat-surface walking twice a day keeps the sciatic nerve gliding through its pathway, reduces disc pressure compared to sitting, and maintains the load cycling that nourishes disc tissue. Start short. Increase only when walking doesn’t worsen symptoms.
4. Piriformis foam rolling
If the pain lives more in the buttock than the lower back, or sitting triggers it more than standing, try foam rolling the piriformis. Sit on a firm ball or roller positioned under one buttock. Find the sore spot. Hold steady pressure for 30–60 seconds per side. Not dramatic relief — but cumulative over several days, it meaningfully reduces piriformis tension when paired with stretching.
Full comparison
| Method | Best For | Speed | Duration | Notes |
|---|---|---|---|---|
| Ice pack | Acute flare, first 72 hrs | Fast | Short-term | Wrap in cloth, 15–20 min |
| Heat pad | After 72 hrs, muscle tightness | Moderate | Short-term | Don’t use during acute phase |
| Gentle walking | Nerve mobility, disc nutrition | Gradual | Cumulative | 10–20 min, flat surface |
| Piriformis foam roll | Buttock-based or sitting-triggered pain | Gradual | Cumulative | Pair with stretching |
| Targeted stretching | Piriformis and hamstring tightness | Moderate | Cumulative | Daily is better than occasional |
What Are the Best Stretches for Sciatic Nerve Pain?
Stretches work by relieving mechanical pressure on the sciatic nerve — either by releasing the piriformis directly, or by decompressing the lumbar segments where disc compression presses on the nerve root.

The key is understanding why certain stretches work. The piriformis is an external rotator of the hip. When you stretch the hip into external rotation, you directly target the muscle most likely compressing the nerve. Generic back stretches that don’t involve external hip rotation do far less for sciatica specifically.
1. Figure-4 stretch
- Lie on your back, both knees bent
- Cross right ankle over left knee
- Gently pull the left thigh toward your chest
- Hold 30–45 seconds on each side
Most accessible stretch for most people. Directly targets piriformis tightness.
2. Knee to opposite shoulder
- Lie flat, legs extended
- Bend the right knee, and clasp hands around it
- Gently pull toward your left shoulder
- Hold 30 seconds, then switch
Releases the gluteal and piriformis muscles simultaneously.
3. Seated spinal twist
- Sit on the floor, legs extended
- Bend right knee, plant foot outside the left knee
- Twist torso right, left elbow on the outside of right knee
- Hold 30 seconds per side
Creates decompression in the lower lumbar segments. Particularly useful for disc-related sciatica.
4. Standing hamstring stretch
- Place the right foot on a low surface — a step or chair
- Flex your foot upward
- Lean forward gently without rounding the back
Tight hamstrings increase tension along the entire sciatic pathway. This stretch is easy to skip. It’s more important than it looks.
What most people get wrong
A stretch should create a pulling sensation in the muscle, not nerve symptoms. If a position increases shooting pain down the leg or causes new numbness, stop. Forcing a stretch into active nerve pain can set recovery back by days.
Quick Takeaway: External hip rotation stretches — figure-4, knee-to-shoulder — target the piriformis directly. Generic back stretches often don’t.
What Helps Sciatic Nerve Pain at Night?
Night pain with sciatica is extremely common. Almost no mainstream health content addresses it specifically.
Sleep position has a direct effect on nerve compression. Lying flat on your back with legs fully extended increases lumbar lordosis — the inward curve of the lower spine — and can push herniated disc material further into the nerve root. Changing position alone can significantly reduce nighttime pain.
Best sleep positions
Option 1 — Side-lying on the non-painful side. Place a pillow between your knees. This reduces lumbar rotation and lowers tension on the sacroiliac joint and nerve root.
Option 2 — Back-lying with a pillow under your knees creates slight hip flexion. Flattens the lumbar curve. Reduces intradiscal pressure.
What to avoid
Sleeping on the painful side narrows the foraminal opening — the channel where the nerve exits the spine — on the affected side. Most people find that this reliably makes the night worse.
One underused fix
An adhesive heat patch on the lower back before bed. The steady, low-level warmth over several hours reduces overnight muscle guarding that builds up around the nerve. This is the source of a lot of morning stiffness.
For medication, naproxen sodium taken with food in the evening has a longer working window than ibuprofen and carries relief further into the early morning hours.
Quick Takeaway: Sleep position and a heat patch before bed are two of the most underused, highest-impact changes for night pain.
Read Related Content
- Is Heat or Ice Better for Nerve Pain? What Science Says!
- 5 Best Exercises for Sciatic Nerve Pain Relief At Home.
- How to Alleviate Sciatic Nerve Pain Naturally.
- Best Thing For Sciatic Nerve Pain: At Home What Really Work?
- How To Reduce Neuropathy Pain Naturally. 7 Remedies Methods.
What Helps Sciatic Nerve Pain in the Morning?
Morning is often the worst part of the day. There’s a specific reason for it.
During sleep, intervertebral discs slowly reabsorb fluid. By the time you wake up, the discs are slightly more expanded than they were the night before. In a spine with a bulging disc, this means increased pressure on an already irritated nerve root. People with disc-related sciatica often feel significantly worse for the first 20–30 minutes after waking, then gradually improve as movement normalizes disc pressure.
What most people do wrong
They stand up abruptly and immediately bend forward. That combination — expanded disc tissue plus forward flexion — maximizes compression on the nerve root at exactly the moment it’s most vulnerable. Most acute morning sciatica flares happen within the first five minutes of getting out of bed.
Morning sequence before getting up
- While still lying down: 5–10 slow knee-to-chest pulls on each side
- Supine spinal twist — both knees bent, drop them slowly to one side, hold 20 seconds, switch
- Roll to your side before sitting up — use your arms to push up, not a straight crunch
- Sit at the edge of the bed for 30 seconds before standing
- Walk slowly for 2–3 minutes before bending, reaching, or lifting anything
Takes less than five minutes. Meaningfully reduces the severity of morning flare-ups.
Quick Takeaway: Disc expansion overnight is the reason morning pain is worse. A brief movement routine before standing changes this significantly.
What Helps Sciatic Nerve Pain During Pregnancy?
Pregnancy sciatica is different from the standard version, and the treatment options are narrower.
The cause is layered. The hormone relaxin loosens spinal and pelvic ligaments, creating joint instability and more room for nerve compression. The growing uterus can directly press on the sciatic nerve as it passes through the pelvis. Shifting weight distribution also changes lumbar curvature and pressure patterns on the disc.
What actually helps
- Physical therapy — the single best option. A skilled PT can assess pelvic alignment and design exercises appropriate for each trimester
- Sacroiliac joint belt or maternity support band — stabilizes the pelvis, reduces nerve tension during walking
- Warm (not hot) baths or a heat pack on the lower back and buttocks
- Prenatal massage from a licensed therapist with pregnancy-specific training
- Figure-4 and knee-to-chest stretches modified for side-lying, not flat on the back in the later trimesters
What to avoid
Ibuprofen and naproxen are not safe during pregnancy — particularly in the third trimester, where NSAID use has been linked to premature closure of the ductus arteriosus. Acetaminophen is the only widely recommended OTC pain option. It addresses pain perception rather than inflammation, which limits its effectiveness, but it’s the appropriate choice here.
Most pregnancy sciatica resolves after delivery as hormone levels normalize and mechanical pressure lifts. The condition is self-limiting, which doesn’t make the third trimester any easier to get through, but it does matter for context.
What Doesn’t Work as Well as People Think
Strict bed rest
A day of rest during a severe acute flare is reasonable. Several days of lying still because it hurts to move likely makes the underlying problem worse — less disc nutrition, more muscle guarding, deeper nerve sensitization.
Sitting and waiting it out at a desk
Prolonged sitting increases intradiscal pressure more than standing or walking. People who develop sciatica at a desk job often need more movement, not less — standing briefly and changing position every 30–45 minutes, not staying seated all day in a soft chair.
Heavy stretching on day one
Forcing a deep stretch session during an acute flare can aggravate the nerve root. The piriformis and surrounding muscles are already inflamed and guarding. Brief, gentle movement during the first 48 hours is fine. Aggressive sessions are not.
Epidural steroid injections as a first step
A systematic review in the Annals of Internal Medicine found mixed results for epidural corticosteroid injections — some short-term pain reduction, but no significant long-term benefit over placebo in multiple analyses.
Injections are a reasonable option after conservative management has failed at 6–8 weeks. Before that point, the evidence does not support them over physical treatment.
Quick Takeaway: The most common mistakes — resting too long, sitting all day, stretching too hard too early — all make nerve pain worse for the same reason: they increase pressure or sensitization on the nerve rather than relieving it.
When Should You See a Doctor for Sciatica?
Sciatica clears with home treatment for most people within 4–12 weeks. There are situations where waiting is the wrong call.
See a doctor promptly if you have:
- Loss of bladder or bowel control — this can indicate cauda equina syndrome, a medical emergency
- Foot drop — weakness or inability to lift the front of the foot when walking
- Symptoms in both legs simultaneously
- Sciatica with fever
- Pain that consistently wakes you from sleep and doesn’t respond to position changes
- No meaningful improvement after 6–8 weeks of consistent home treatment
As of 2026, current guidance from the American Academy of Orthopaedic Surgeons holds that surgery is appropriate only when symptoms are severe, persistent, and accompanied by measurable neurological deficits. Most people with sciatica never reach that threshold.
Frequently Asked Questions
How long does sciatic nerve pain last?
Most cases resolve within 4 to 12 weeks with conservative treatment, including movement, stretching, and anti-inflammatory medication. Some cases persist longer, particularly when caused by a significant disc herniation. If symptoms have not improved meaningfully after 6 to 8 weeks of home treatment, seeing a doctor to identify structural causes is worth doing.
Is it better to rest or walk with sciatic nerve pain?
Walking is generally better than resting in most cases. Gentle movement keeps the nerve mobile and prevents the defensive muscle guarding that deepens the pain cycle. A Cochrane review found that staying active was at least as effective as bed rest for acute sciatica. Short walks on flat terrain are ideal, particularly in the first few days.
What is the fastest way to relieve sciatic nerve pain?
The fastest short-term relief usually combines an oral NSAID, an ice pack applied to the lower back or buttock for 15 to 20 minutes, and a figure-4 stretch held 30 seconds per side. For pain triggered by prolonged sitting, simply standing and walking slowly for a few minutes often produces immediate relief.
Can sciatic nerve pain go away on its own?
Yes, in most cases. Research consistently shows 80 to 90 percent of people recover without surgery, typically within 6 to 12 weeks. Gentle activity and basic anti-inflammatory management are enough for most people. Sciatica that persists beyond three months, or involves weakness or loss of bladder and bowel control, warrants medical evaluation.
What OTC medicine is best for sciatic nerve pain?
Naproxen sodium (Aleve) is often the most practical choice because its 8 to 12-hour duration covers nighttime better than ibuprofen’s shorter window. Ibuprofen works well for daytime management, taken every 6 to 8 hours. Acetaminophen is less effective for sciatica because it does not reduce inflammation, which drives most cases.

Recent Posts