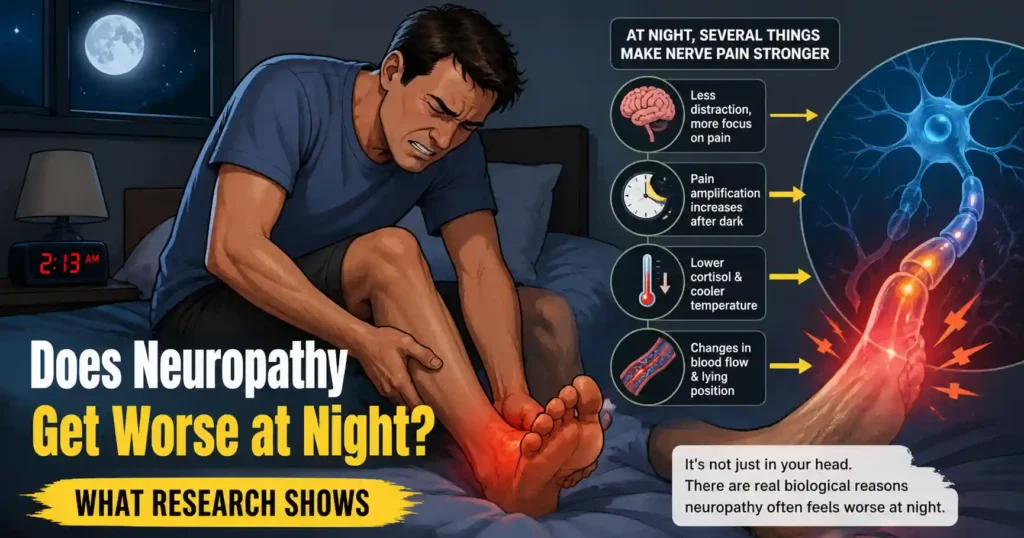
If you are also wondering, “Does Neuropathy Get Worse at Night?” then the simple answer is, Yes — neuropathy genuinely gets worse at night. It is not just that the quiet makes pain harder to ignore. Multiple biological processes peak after dark that amplify nerve pain signals and weaken the body’s ability to suppress them at the same time.
A study from the Comprehensive Pain Center at Oregon Health & Science University, tracking nearly 650 patients with diabetic peripheral neuropathy, confirmed that peak pain consistently falls between 11 pm and 8 am.
Key Takeaways
- Neuropathy is biologically worse at night — pain amplification rises while the body’s natural pain suppression drops after dark.
- Gate control theory explains the daytime relief — movement and sensory input help “close” the spinal pain gate; lying still opens it.
- Cortisol drops to its lowest level near midnight — this increases inflammation around damaged nerves, a factor most articles ignore.
- Cold temperatures disrupt damaged nerves — slower nerve conduction leads to irregular firing, felt as burning or sharp pain.
- Diabetic peripheral neuropathy shows the strongest night pattern — observed across nearly 650 patients in the OHSU study.
- “Neuropathy only at night” is a real condition — often linked to early small fiber neuropathy and allodynia, not imagined symptoms.
Does Neuropathy Actually Get Worse at Night, or Does It Just Feel That Way?
It gets worse. Two separate mechanisms fire simultaneously after dark:
- Pain signals become louder — damaged nerves transmit more abnormal firing with less interference
- Pain suppression weakens — your brain’s filtering system runs at reduced capacity overnight
This explains why some people have manageable daytime symptoms but severe nighttime pain from the same nerve damage. The nerves aren’t more damaged at night. The body is simply worse at blocking what they send.

During the day, movement, conversation, and sensory input from the environment feed competing signals into your nervous system. Those signals partially crowd out the noise from damaged nerves. Lie still in a quiet room, and that noise has nothing to compete with.
Quick Takeaway: Nighttime neuropathy worsening is biological, not psychological — both pain amplification and pain suppression loss occur at the same time after dark.
What Happens to Pain Signals After Dark?
The gate control theory of pain (Melzack & Wall, Science, 1965) describes how the spinal cord acts as a gatekeeper. Sensory input from daily activity partially closes that gate. Stillness opens it.
At night, two biochemical changes compound this:
- Norepinephrine and serotonin drop. Both neurotransmitters help dampen pain signals from peripheral nerves. As the body prepares for sleep, levels of both fall — and damaged nerves transmit with less filtration as a result.
- Cortisol hits its daily low. Cortisol is naturally anti-inflammatory and peaks around 6–8 am. By midnight, it is near its lowest point. That drop means inflammatory activity around damaged nerves increases precisely during sleep hours.
This cortisol angle gets almost no coverage in standard neuropathy content, which is odd. For anyone with diabetic or inflammatory neuropathy, the overnight cortisol trough is likely a significant driver of nighttime flares — not just body position or room temperature.
Why Does Cold Air Make Nerve Pain Spike at Night?
Cold is the most common nighttime trigger for neuropathy pain. The usual explanation is “cold makes nerves more sensitive.” True — but the actual mechanism is more specific.
Damaged peripheral nerves already have reduced nerve conduction velocity — the speed at which electrical signals travel along the fiber. When the temperature drops, that velocity slows further. For healthy nerves, this is minor.

For damaged nerves already below normal threshold, the slowdown triggers abnormal signal bursts — and the brain reads those bursts as burning, tingling, or sharp pain.
Your core body temperature drops during sleep. Your thermostat may be lower. Blankets rarely cover feet the way they cover your torso. These compounds.
Feet and hands are hit hardest because they are furthest from the heart, have the least insulating tissue, and cool the fastest.
According to Loma Linda University Health, people with peripheral neuropathy show measurably greater pain responses to temperature changes than the general population, not just greater discomfort.
Why Is Diabetic Neuropathy Especially Worse at Night?
Diabetic peripheral neuropathy follows the nighttime worsening pattern more sharply than most other types. The OHSU study confirmed the 11 pm–8 am peak across all patients, but the effect was most consistent in diabetic cases.
Several factors drive this:
- Blood sugar fluctuations overnight — particularly nocturnal hypoglycemia in people on insulin — can directly destabilize nerve function during sleep
- Small fiber nerve damage — the fibers diabetes targets first are the same ones that generate burning and shooting pain, most acutely felt when lying still
- Reduced overnight circulation — autonomic nerve damage from diabetes impairs blood flow to the extremities, worsening the metabolic stress on already-compromised nerve tissue
There is also a sleep architecture problem. A 2010 study in Pain found that pain disrupts sleep and disrupted sleep lowers the pain threshold — a bidirectional cycle.1Sleep deficiency and chronic pain: potential underlying mechanisms and clinical implications, PubMed Central. For diabetic neuropathy patients, this cycle can become self-reinforcing in ways that are genuinely hard to interrupt without targeted treatment.
Quick Takeaway: Diabetic neuropathy worsens at night due to blood sugar instability, small fiber vulnerability, and reduced circulation — stacked on top of the biological pain-amplification changes that affect all neuropathy types.
Why Does Neuropathy Sometimes Only Happen at Night?
Some people have no neuropathy symptoms during the day — only at night. This distinct pattern gets no coverage in standard articles on this topic, but it is common enough to need an explanation.
The most likely cause is small fiber neuropathy in early or mild stages. During the day, physical movement generates enough sensory input to keep the spinal pain gate partially closed. Even a small number of damaged, misfiring fibers can be masked by that background activity.
At night, with no competing signals, those same few fibers can generate noticeable — sometimes severe — symptoms.
People with this pattern are often told their neuropathy is mild, which may be clinically accurate. But “mild” does not capture waking up at 2 am with burning feet.
Allodynia is also more pronounced at night for this reason. Allodynia is pain caused by stimuli that should not be painful — the weight of a sheet, the contact of a sock.
Damaged nerves become hypersensitive to any input when background sensory stimulation drops. If your sheets feel unbearable at night but your feet feel normal during the day, allodynia is likely the reason.
What Can You Do to Reduce Nighttime Neuropathy Pain?
No single approach works for everyone. The options with practical backing address specific mechanisms — not general wellness advice.
| Cause | Mechanism | What Helps | Who It Helps Most |
|---|---|---|---|
| Distraction loss / gate opens | Pain signals reach brain unfiltered | White noise; TENS device before bed | Anyone with neuropathy |
| Temperature drop | Nerve conduction slows, abnormal firing increases | Loose warm socks; room at 68–70°F; lightweight heated blanket | Foot and hand neuropathy |
| Cortisol trough / inflammation rise | Inflammatory activity peaks near midnight | Consistent sleep schedule; anti-inflammatory diet | Diabetic and inflammatory neuropathy |
| Nerve compression from sleep position | Body weight compresses peripheral nerves | Pillow between knees (side sleepers); pillow under legs (back sleepers) | Lower extremity and lumbar neuropathy |
| Fatigue lowering pain threshold | Exhaustion reduces pain suppression capacity | Morning or afternoon exercise — not evening | Chronic fatigue patterns |
| Medication levels dropping overnight | Short half-life drugs lose potency by bedtime | Discuss dose timing with your prescribing doctor | People on gabapentin or pregabalin |
On medication timing: Gabapentin and pregabalin have short half-lives. A single morning dose may leave serum levels genuinely low by 10 pm. This is a fixable problem — but it requires a physician conversation about redistribution, not independent adjustments.
On temperature: The goal is warmth without weight. A heavy blanket on the feet with allodynia adds the compressive stimulus that triggers pain. Lightweight microfiber or loose thermal socks achieve warmth without pressure.
On exercise: Research by Younger et al. (Pain, 2010) found that physical exhaustion lowers pain threshold in chronic pain conditions. Evening exercise, healthy for most people, may work against neuropathy patients specifically.2Exercise-Induced Hypoalgesia in Pain-Free and Chronic Pain Populations: State of the Art and Future Directions, ScienceDirect. Morning or early afternoon is the practical adjustment most clinicians don’t mention.
Related Articles
- For a closer look at the nutritional and nerve-support factors that affect how neuropathy progresses and responds to treatment, read our detailed analysis about Arialief.
Frequently Asked Questions
Why does foot neuropathy get worse at night?
Feet cool the fastest because they are furthest from the heart and have little insulating tissue. Cooler temperatures slow nerve conduction velocity in already-damaged fibers, causing abnormal signal bursts that the brain reads as pain. Walking during the day also partially closes the spinal pain gate — lying still at night removes that suppression entirely.
Does neuropathy pain actually get worse overnight, or does it just feel that way?
It actually gets worse. Pain-suppressing neurotransmitters — norepinephrine and serotonin — drop as you approach sleep. Anti-inflammatory cortisol also hits its daily low near midnight. Your nervous system is genuinely less able to filter pain signals during these hours, not only less distracted from them.
Why is diabetic neuropathy worse at night than other types?
Diabetic neuropathy targets small fiber sensory nerves — the fibers responsible for burning and shooting pain. These nerves are sensitive to blood sugar fluctuations and reduced overnight circulation, both of which are worse during sleep in diabetic patients. The cortisol trough and slowed circulation compound an already vulnerable nerve environment.
Can sleeping position make neuropathy pain worse?
Yes. Sustained body weight on one side puts prolonged pressure on peripheral nerves near the hip, knee, and ankle. For someone with existing nerve damage, this can trigger or worsen pain within minutes of lying down. Sleeping on your back with a pillow under the knees, or on your side with a pillow between the knees, meaningfully reduces this pressure.
What helps stop neuropathy pain at night?
As of 2026, the most practically supported approaches are: warming the feet with loose socks, repositioning to reduce nerve compression, using white noise to partially restore the spinal pain gate, and — for people on gabapentin or pregabalin — discussing dose timing with a physician. If nighttime pain is severe despite these steps, early small fiber neuropathy evaluation and a medication review are the two most frequently overlooked clinical next steps.
Scientific References
- 1Sleep deficiency and chronic pain: potential underlying mechanisms and clinical implications, PubMed Central.
- 2Exercise-Induced Hypoalgesia in Pain-Free and Chronic Pain Populations: State of the Art and Future Directions, ScienceDirect.

Recent Posts