Constipation relief during pregnancy means using safe methods to improve bowel movement frequency and ease stool passage while hormonal and physical changes slow digestion. It mainly focuses on correcting slow gut movement, stool dryness, and pressure from the growing uterus. Most cases are manageable with diet, timing, movement, and, when needed, safe medical options.
Key Takeaways
- Constipation is caused by hormones, iron, and pressure—not just diet
- Fiber alone doesn’t fix it—hydration and movement matter
- Iron supplements are a major hidden cause
- Morning routine (warm fluid + movement) works better than random fixes
- The third trimester needs gentler strategies
- Medication is useful—but not the first step
What Is Constipation Relief During Pregnancy?
Constipation relief during pregnancy is not just about “going more often.” It’s about fixing how your digestive system is functioning under hormonal pressure.
During pregnancy, bowel movements slow down. Stool sits longer in the colon. More water gets absorbed. That’s why stools become hard and difficult to pass.
Relief strategies aim to:
- Soften stool
- Improve gut movement
- Reduce strain
Here’s what most articles get wrong: they treat all constipation the same. It isn’t. The cause determines what actually works.
Quick Takeaway: Constipation relief is about fixing slow digestion and hard stool—not just forcing a bowel movement.
Why Do Pregnant Women Get Constipated?
Pregnancy constipation is driven by three main mechanisms, not just “hormones.”
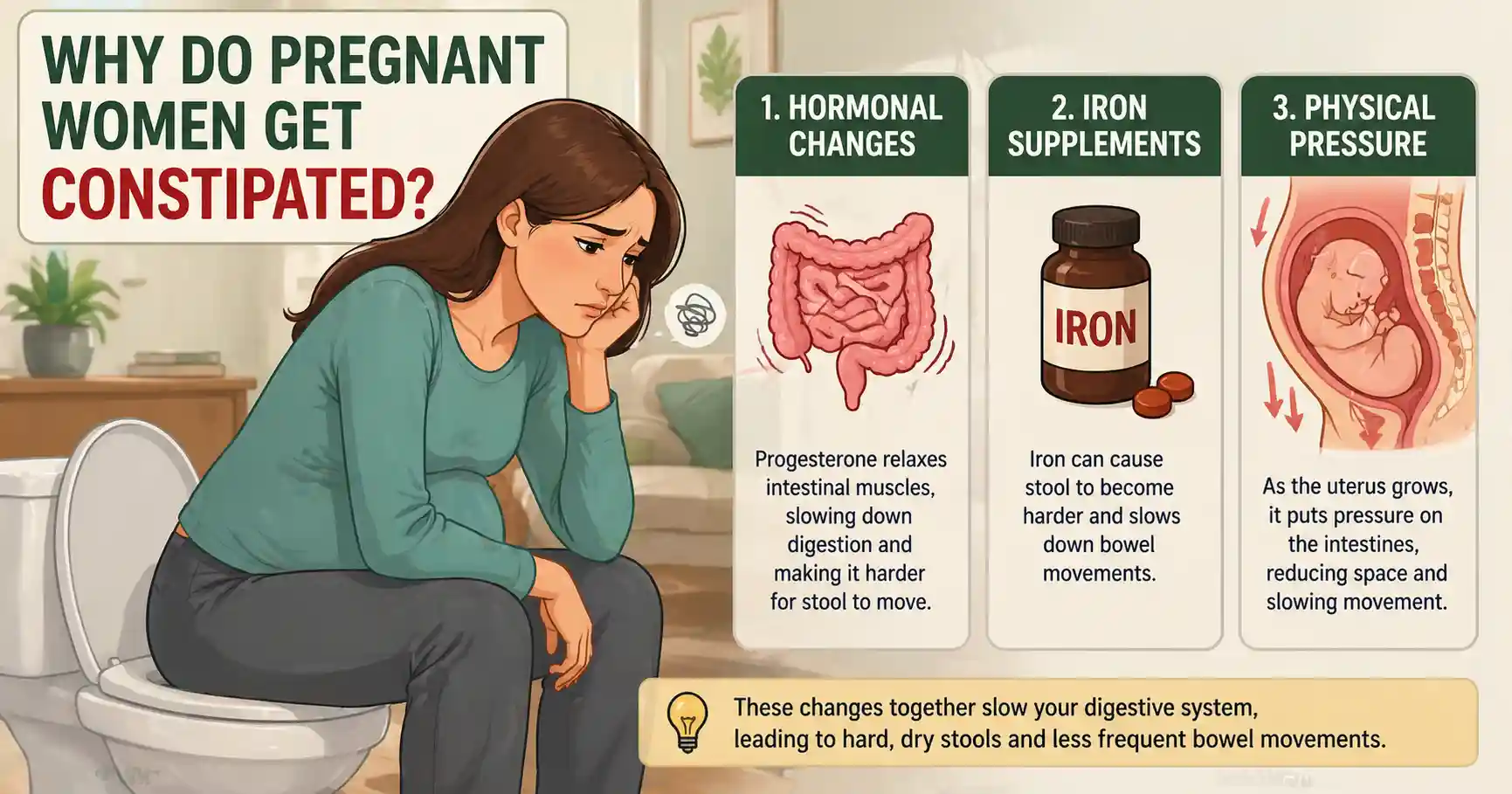
1. Progesterone Slows the Gut
Progesterone relaxes smooth muscles. That includes your intestines.
Result: food moves more slowly → more water absorbed → harder stool
2. Iron Supplements Make Stool Harder
Many prenatal vitamins contain iron. Iron:
- Slows bowel movement
- Darkens and hardens stool
This is one of the most overlooked causes.
3. Physical Pressure From the Uterus
As pregnancy progresses:
- The uterus presses on the intestines
- Movement becomes restricted
This is why constipation often worsens in later trimesters.
A 2023 review from the Cleveland Clinic confirms that up to 40% of pregnant women experience constipation, mainly due to these combined effects.
What stood out in research: iron-related constipation is often stronger than hormonal effects, but most content barely mentions it.
Quick Takeaway: Constipation isn’t random—it’s driven by hormones, iron, and physical pressure.
How to Relieve Constipation During Pregnancy Fast
Fast relief depends on matching the fix to the cause. Blindly adding fiber often backfires.

What Actually Works (Ranked by Effectiveness)
| Method | When It Works Best | Why It Works |
|---|---|---|
| Warm fluids (morning) | Slow gut movement | Triggers bowel reflex |
| Walking (10–20 mins) | Sluggish digestion | Stimulates intestinal motion |
| Magnesium-rich foods | Hard stool | Helps relax bowel muscles |
| Fiber (controlled amount) | Low fiber intake | Adds bulk, but needs water |
| Stool softeners | Severe cases | Directly softens stool |
Immediate Relief Steps (Same-Day Impact)
- Drink warm water after waking up
- Walk for 10–15 minutes
- Eat a small fiber source (like soaked chia or fruit)
- Don’t delay the urge
That last one matters more than people think. Ignoring the urge trains your body to suppress signals.
Where Most Advice Fails
- Too much fiber without water → worse bloating
- Water alone → useless if gut is slow
- No movement → nothing stimulates bowel reflex
A study in the American Journal of Gastroenterology (2015) found that fiber improves stool frequency only when paired with adequate hydration and movement. Alone, the results were inconsistent.
Quick Takeaway: Fast relief comes from combining hydration, movement, and timing—not one single fix.
What Can Pregnant Women Safely Take for Constipation?
Medication should be the last step, not the first move.
Generally Considered Safe Options
- Stool softeners (like docusate)
- Bulk-forming agents (psyllium husk)
- Osmotic laxatives (polyethylene glycol, under guidance)
The American College of Obstetricians and Gynecologists supports these when lifestyle changes fail.
What to Avoid
- Stimulant laxatives (frequent use)
- Herbal “detox” products
- Castor oil (can trigger contractions)
Hard Truth
Most people jump to supplements too early. Fix the basics first. Medication works better when the underlying cause is addressed.
Quick Takeaway: Safe options exist, but they work best after fixing diet and movement.
What Foods Actually Help With Constipation During Pregnancy?
Not all “fiber foods” are equal. Some help. Some make things worse.
Foods That Actually Work
- Prunes – contain sorbitol, a natural laxative
- Oats – soluble fiber, easier on digestion
- Kiwi – improves stool frequency (clinical evidence supports this)
- Flaxseeds – add bulk + lubrication
- Vegetables (cooked) – easier than raw for many women
Foods That Often Backfire
- Raw salads (hard to digest)
- Excess bran (can cause gas and a feeling of blockage)
- Processed “fiber bars.”
The Real Rule
Fiber must be:
- Gradual
- Paired with water
- Matched to your tolerance
A 2020 NIH-backed review showed that sudden high fiber intake increases bloating without improving stool frequency in many cases.
Quick Takeaway: The right fiber helps. Too much or the wrong type makes things worse.
What Makes Constipation Worse During Pregnancy?
Some habits quietly make the problem worse.
Common Triggers
- Ignoring the urge to go
- Low physical activity
- High iron intake without balance
- Dehydration
- Sudden diet changes
Non-Obvious Insight
Timing matters more than quantity.
Example:
- Drinking 3 liters randomly ≠ helpful
- Drinking warm fluid in the morning → triggers bowel reflex
That’s the difference most content ignores.
Quick Takeaway: It’s not just what you eat—it’s how and when you do it.
Constipation Relief During 3rd Trimester: What Changes
Third-trimester constipation is harder to manage. That’s just reality.
What Changes
- More uterine pressure
- Reduced movement
- Slower digestion
What Works Better Here
- Smaller, frequent meals
- Gentle daily walking
- Stool softeners (if needed)
- Avoiding heavy, bulky meals
What Stops Working Well
- High-fiber overload
- Large meals
- Long periods of sitting
This is where many women get frustrated. The same tricks from early pregnancy stop working.
Quick Takeaway: Third-trimester constipation needs gentler, more frequent adjustments—not aggressive fixes.
Exercises That Help Constipation During Pregnancy
You don’t need a workout plan. You need consistent movement.
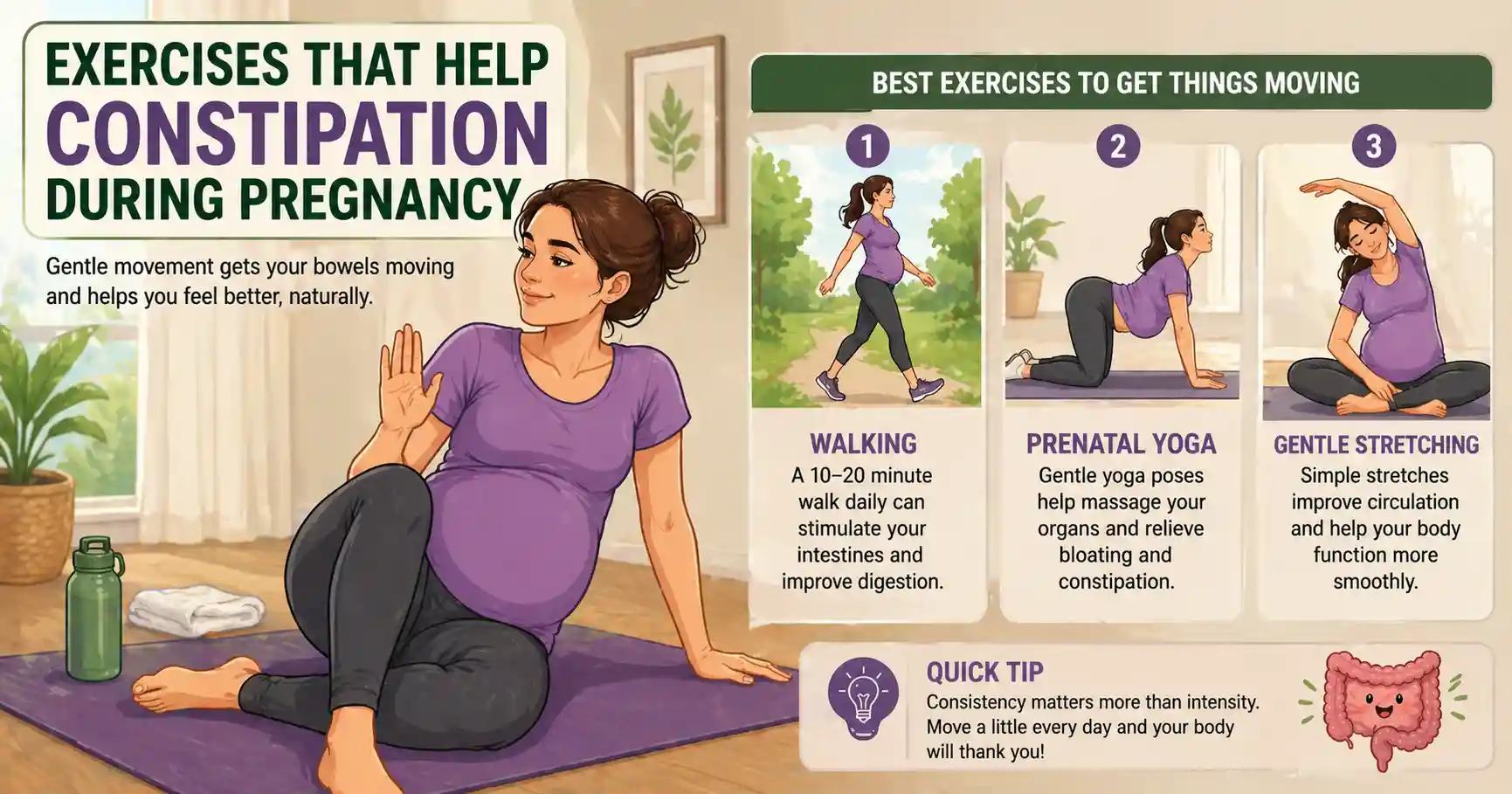
Effective Options
- Walking (10–20 minutes daily)
- Prenatal yoga
- Light stretching
Why It Works
Movement:
- Stimulates intestinal contractions
- Reduces stagnation
- Improves blood flow to digestive organs
What Doesn’t Work
- Intense workouts (not sustainable)
- Sitting all day and “compensating later.”
Consistency beats intensity.
Quick Takeaway: Regular movement is one of the simplest and most reliable fixes.
When Is Constipation Dangerous During Pregnancy?
Most cases are harmless. Some are not.
Warning Signs
- Severe abdominal pain
- Blood in stool
- No bowel movement for several days
- Vomiting with constipation
These may indicate:
- Fecal impaction
- Obstruction
- Other complications
If symptoms persist, seek medical help. Guessing here is a bad idea.
Quick Takeaway: Mild constipation is common. Severe or painful cases need evaluation.
FAQs
How to relieve constipation while pregnant quickly?
Start with warm fluids in the morning, followed by light movement like walking. Add a small amount of fiber, such as fruit or oats. Avoid large meals and don’t ignore the urge to go. Quick relief depends on combining hydration, movement, and timing, not just one method.
Is constipation safe during pregnancy?
In most cases, yes. It is common due to hormonal and physical changes. However, severe symptoms like pain, bleeding, or prolonged constipation need medical evaluation. Ignoring persistent symptoms can lead to complications such as hemorrhoids or fecal impaction.
What can pregnant women take for constipation safely?
Stool softeners, bulk-forming agents, and some osmotic laxatives are generally considered safe under medical guidance. Lifestyle changes should always come first. Medication works best when combined with proper hydration, diet, and physical activity.
Why does constipation get worse in the third trimester?
The growing uterus puts more pressure on the intestines, slowing movement further. Physical activity often decreases, and digestion slows down further. These combined factors make constipation harder to manage compared to earlier stages of pregnancy.
Final Word
Constipation relief during pregnancy isn’t about throwing random remedies at the problem. It’s about understanding what’s causing it in your body and fixing that specifically. That’s where most advice fails—and why people stay stuck longer than they should.

Recent Posts