Sciatic nerve pain doesn’t feel like normal back pain. It feels sharper. Stranger. And it doesn’t stay in one place.
Most people first notice it when pain starts in the lower back or hip and then shoots down one leg. Sometimes it feels like a quick electric shock. Other times it’s a slow-burning line that runs from your butt to your calf. You might also feel tingling in your foot or even numbness that doesn’t go away when you move.
That happens because this is a nerve problem, not a muscle problem. The sciatic nerve runs from your lower spine all the way down to your foot. When something presses on it, the signal changes along the whole path. That’s why the pain travels instead of staying in one spot.
Here’s where most people mess up. They treat it like a pulled muscle. They lie down more. They stretch randomly. Or they just wait it out. That usually slows things down. Sometimes it makes it worse.
What research shows is more specific. Guidance from the Mayo Clinic (2023) and the Cleveland Clinic (2024) points to one main issue—pressure on a nerve, often from a disc in the lower back. But that’s not the full story. Studies, including work in The Lancet Rheumatology (2020), show that inflammation around the nerve also plays a role. That’s why the pain can feel strong even when the physical damage looks small.
And here’s something science still hasn’t fully figured out. Two people can have the same disc problem on a scan, but one feels severe pain, and the other barely notices it. So pain level doesn’t always match damage level. That’s frustrating, but it’s real.
In this guide, we’re not just naming the problem. We’re breaking it down in a way you can actually use. What does the pain mean? How to tell if it’s really sciatica. And what actions help based on how your pain behaves day to day.
| Field | Details |
|---|---|
| What it is | Sciatic nerve pain happens when a nerve in your lower back gets irritated or compressed, and the pain travels down your leg |
| What people claim | Most people think rest and a few stretches will fix it |
| What research says | Staying active in the right way works better than staying still, especially after the first few days |
| Biggest benefit | The right movement can reduce pressure on the nerve and make daily movement easier |
| Biggest limitation | Wrong exercises or too much rest can increase nerve irritation and drag recovery out |
| Best for | People with mild to moderate symptoms who can still walk and move without severe weakness |
| Be careful if | You notice growing numbness, trouble lifting your foot, or any loss of bladder or bowel control |
| Bottom line | Sciatic nerve pain usually gets better, but not by guessing. The way your pain behaves gives you clues about what’s causing it. If you follow those clues and move the right way, recovery is faster. If you ignore them, it tends to stick around much longer. |
What does sciatic nerve pain feel like in the body?
Sciatic nerve pain feels different from muscle pain. It is sharper, spreads farther, and changes with movement.
It usually starts in the lower back or butt and then moves down one leg. The path is often clear. Back → thigh → calf → sometimes foot. In most cases, only one side is affected. This pattern matters because muscle pain does not travel like this.
Why does it feel sharp, burning, or electric
Sciatic pain comes from a nerve, so the sensation is different.
Muscle pain feels sore and tight. You can press it and find the exact spot. Nerve pain does not behave like that. It feels deeper and harder to locate.
Common sensations include:
- Sharp shooting pain
- Burning along the leg
- Tingling in the foot
- Pins and needles
This is called neuropathic pain. The International Association for the Study of Pain defines it as pain caused by irritation or damage to a nerve.
The reason is signal distortion. A compressed nerve does not send clean signals to the brain. Instead, the signals become irregular. That creates sensations like burning or electric shock without a direct physical cause.
Clinical descriptions from the Mayo Clinic (2023) match this pattern. Patients often describe the pain as shooting or electric rather than dull.
Why does the pain travel down the leg
The pain travels because of how the sciatic nerve is structured.
The nerve starts in the lower spine and runs down the entire leg. When a nerve root is irritated near the spine, the brain interprets the pain along the full pathway.
This is known as referred nerve pain.
A review in The Lancet Rheumatology (2020) explains that nerve root compression leads to pain signals being perceived distally, often far from the actual site of compression.
This explains why:
- A disc problem in the lower back can cause calf pain
- Nerve irritation can lead to foot tingling
The location of pain does not always match the location of the problem.
Why do symptoms change during the day
Sciatic pain changes based on posture because spinal position affects nerve pressure.
When you sit, the lower spine flexes slightly. This increases pressure on the discs. If a disc is pressing on a nerve, sitting can worsen symptoms. This is common in desk work or long driving.
When standing or walking, the spine position changes. In some cases, this reduces pressure. In others, especially spinal stenosis, standing or walking increases symptoms due to reduced space around the nerve.
Typical patterns:
- Sitting for long periods → gradual increase in pain
- Standing after sitting → sudden sharp pain
- Walking long distances → increased pain in stenosis cases
- Slight forward bending → relief in some individuals
The Cleveland Clinic (2024) notes that posture directly affects nerve compression, which explains symptom variation throughout the day.
Key takeaway
Sciatic nerve pain is identified by three main features:
- It travels down one leg
- It feels sharp, burning, or electric
- It changes with posture and movement
These features distinguish it from muscle-related pain and indicate nerve involvement.
How do you know if it’s your sciatic nerve?
You can’t confirm it at home with 100% certainty. But you can look at clear patterns.
Sciatic nerve pain has a few signs that repeat in most people. The pain travels. It affects one side. And it often comes with unusual sensations like tingling or numbness.
Doctors use the same basic clues before ordering tests.
The simplest self-check (straight leg raise logic)
Lie flat on your back. Keep one leg straight. Slowly lift that leg without bending the knee. If this causes pain that shoots down your leg, not just in your back, it points toward nerve irritation.
This test stretches the sciatic nerve. If the nerve is already under pressure, stretching it increases symptoms. That is why the pain appears during this movement.
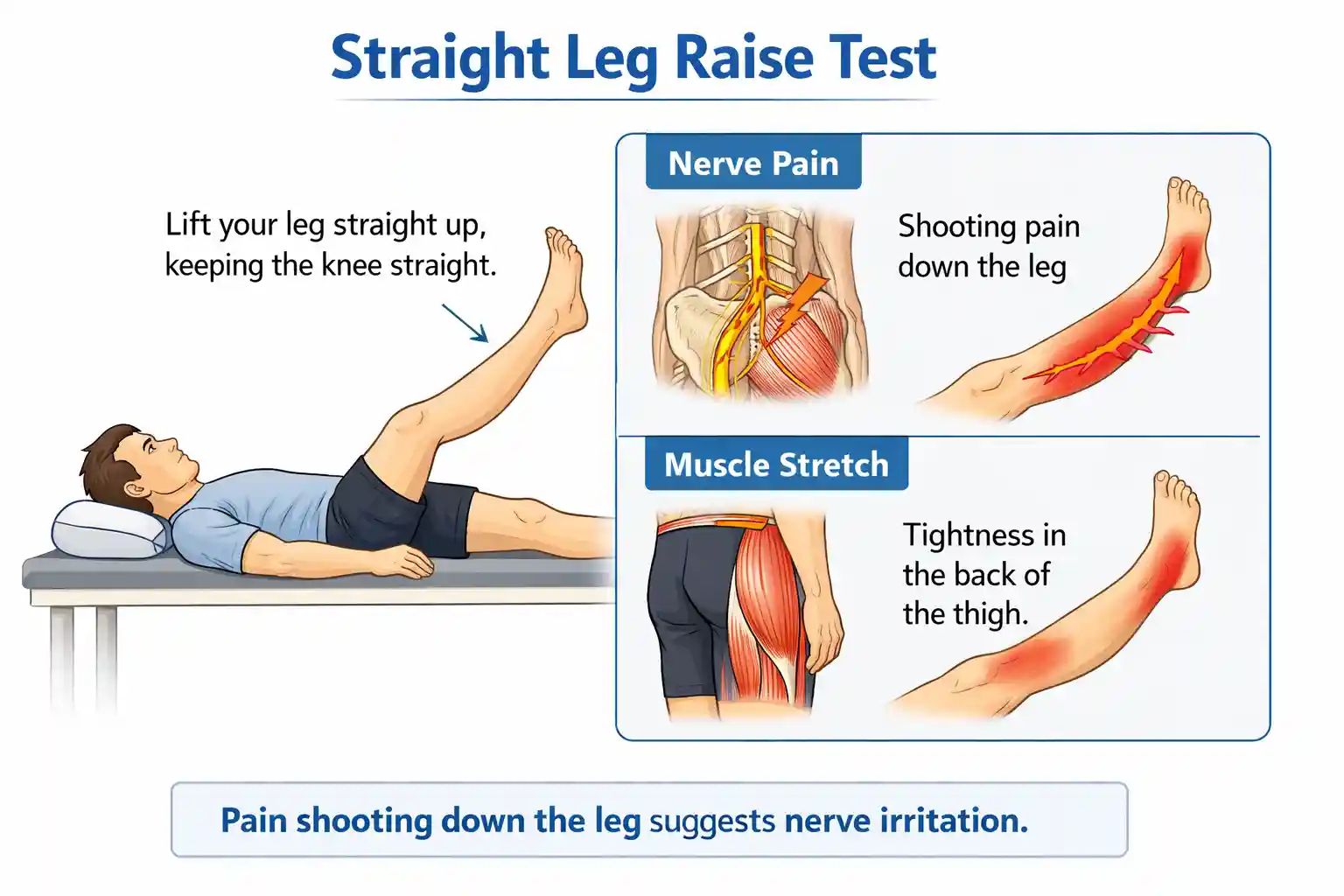
In clinics, this is called the straight leg raise test. It is one of the most common checks used to identify nerve-related pain in the lower back.
If you only feel tightness in the back of your thigh, that is more likely muscle stretch, not nerve pain.
Nerve symptoms vs muscle symptoms
Sciatic nerve pain is not just about pain. It often includes other sensations.
Common nerve-related signs:
- Tingling in the leg or foot
- Numb areas on the skin
- A burning feeling
- Weakness in the leg or foot
Muscle pain is different. It usually feels sore, tight, and stays in one place. It does not cause numbness or tingling.
This difference matters.
If you feel pain along with tingling or numbness, the nerve is likely involved. Muscles do not create those sensations. Weakness is another key sign. If your foot feels heavy or you struggle to lift it while walking, that suggests the nerve is not working properly.
The “travel pattern” test
Sciatic pain follows a path. That is one of the clearest signs.
It usually moves like this: Lower back → butt → back of thigh → calf → sometimes foot
The exact path can vary, but the pattern stays similar. It does not jump randomly from one place to another.
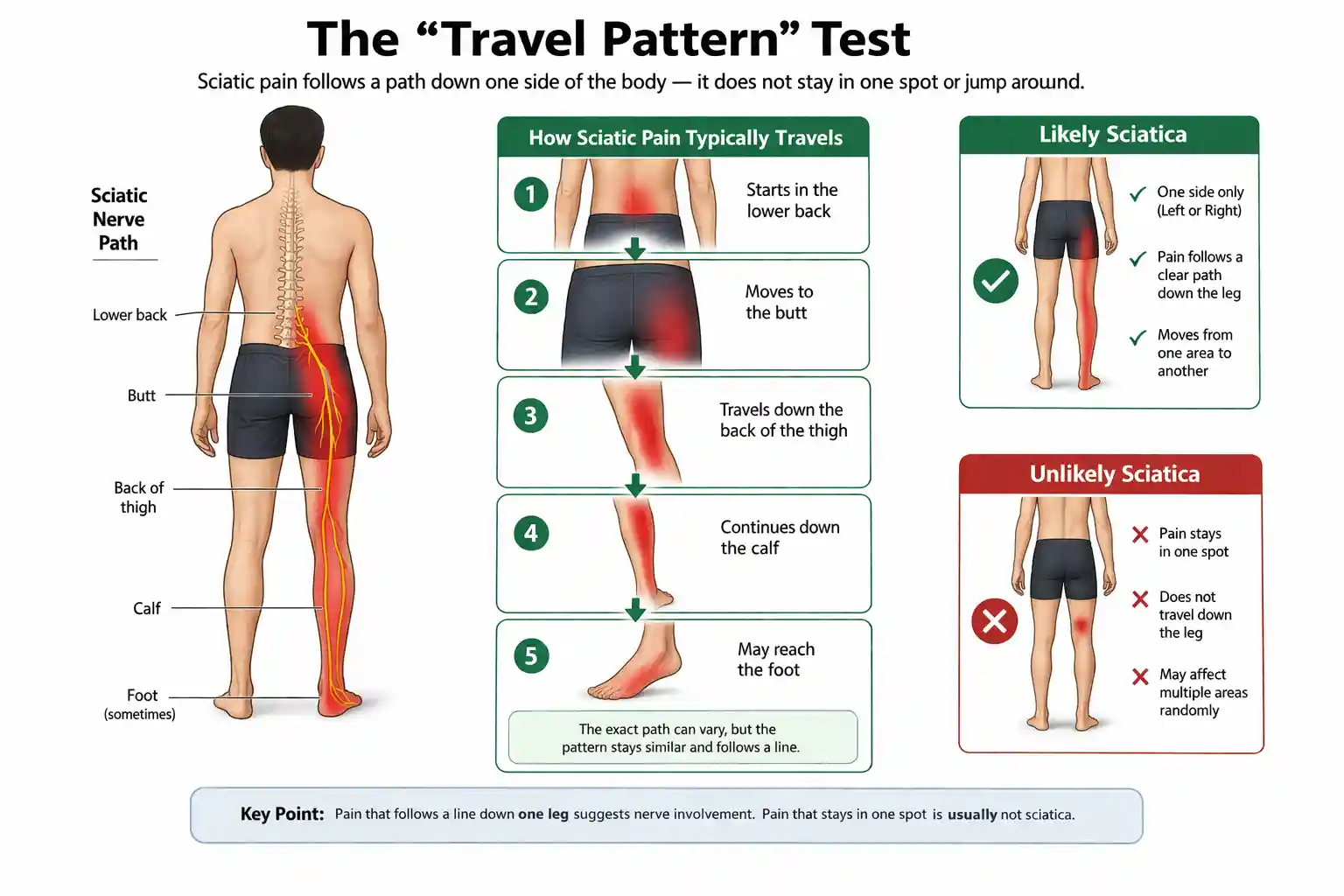
It also usually affects one side of the body. Left or right, not both at the same time. If your pain follows a line down your leg, that strongly suggests nerve involvement.
If your pain stays in one spot, it is likely not sciatica.
What this means
If your pain:
- Shoots down one leg
- Gets worse when you lift your straight leg
- Comes with tingling, numbness, or weakness
There is a strong chance your sciatic nerve is involved.
At that point, treating it like simple muscle pain is usually not enough.
What is mistaken for sciatica pain?
Many conditions feel similar to sciatica. That is why people often misjudge their pain. The key difference is how the pain behaves. Sciatic pain usually travels down the leg. Other conditions tend to stay in one place or follow a different pattern.
Muscle strain (localized vs radiating)
A muscle strain is the most common mix-up. It usually happens after lifting something heavy or sudden movement. The pain stays in one area, often in the lower back or upper thigh.
The feeling is:
- Dull or tight
- Worse when you move or press the spot
- Limited to one small area
It does not travel down the leg. It also does not cause tingling or numbness. If your pain stays in one place, it is more likely a muscle problem.
Piriformis syndrome (hip-based compression)
This condition comes from a small muscle deep in the butt area. The muscle can press on the sciatic nerve. The pain can feel similar to sciatica, but the source is different.
Common signs:
- Pain starts in the butt, not the lower back
- Worse when sitting for long periods
- Pain increases with hip movement
The nerve pain may go down the leg, but it usually does not go as far or as strongly as true sciatica from the spine. This condition is often linked to posture, long sitting, or overuse of the hip muscles.
Spinal stenosis (age-based narrowing)
This is more common in people over 50. In this condition, the space around the nerves becomes narrow. This puts pressure on the nerve roots. The pattern is different from disc-related sciatica.
Common signs:
- Pain increases when walking or standing
- Relief when sitting or bending forward
- Pain may affect both legs in some cases
Many people notice they can walk only a short distance before needing to stop.
Key differences at a glance
| Condition | Trigger | Pain pattern | Age group |
|---|---|---|---|
| Sciatic nerve pain | Disc pressure, nerve irritation | Travels down one leg in a clear path | Common 30–50, but can occur at any age |
| Muscle strain | Lifting, sudden movement | Stays in one spot, does not travel | Any age |
| Piriformis syndrome | Long sitting, hip overuse | Starts in the butt, may spread slightly down the leg | Adults, often active or sedentary workers |
| Spinal stenosis | Walking, standing | Pain increases with walking, better when bending forward | Mostly over 50 |
What this means
The pattern of your pain matters more than the name.
- If the pain stays in one place, it is usually not sciatica.
- If it starts in the butt and links to sitting, it may be muscle-related.
- If it worsens with walking and improves when bending forward, it may be spinal narrowing.
These patterns help guide the next step and prevent wrong treatment.
What actually causes sciatic nerve pain? (Real mechanism)
Sciatic nerve pain starts when a nerve in your lower back gets irritated. This usually happens for two reasons when working together.
Mechanical compression (disc, bone, narrowing)
The most common cause is pressure on the nerve.
This can come from:
- A disc pushing out of place
- Bone growth pressing on the nerve
- Narrow space in the spine
When this happens, the nerve gets squeezed. That affects how signals move through it. This is why pain often starts in the back but shows up in the leg.
Chemical inflammation (nerve irritation)
Pressure is not the full story. When a disc is damaged, it can release chemicals that irritate the nerve. These chemicals increase sensitivity, even if the pressure is small.
Research published in The Lancet Rheumatology (2020) and studies in Spine Journal show that inflammation plays a major role in nerve pain.
This explains why:
- Pain can feel very strong
- Even small disc problems can cause big symptoms
Why does pain feel intense even with small damage
Nerves are sensitive structures. Even mild irritation can create strong pain signals. This is different from muscles, where pain usually matches the level of injury.
That is why some people feel severe pain even when scans show only minor changes.
Why pain does not always match severity
There is often a mismatch between scans and symptoms. Some people have clear disc issues on imaging but feel little pain. Others have severe pain but only small changes on scans.
Studies in the Spine Journal show that imaging does not always predict pain level. This means pain alone does not tell you how serious the condition is.
Why your pain pattern matters more than the diagnosis
The name of the condition matters less than how your pain behaves. Your daily pattern gives better clues than a label.
Disc-related sciatica pattern
Pain usually:
- Gets worse when sitting
- Increases when bending forward
- May improve when standing or walking
This is because sitting increases pressure on the disc.
Stenosis pattern
Pain usually:
- Gets worse when walking or standing
- Improves when sitting or bending forward
This happens because bending forward creates more space for the nerve.
Muscle-related pattern
Pain usually:
- Starts in the butt area
- Gets worse with certain movements or postures
- Often linked to long sitting
- What this means: Use your pain behavior as a guide. How your pain changes with movement often tells you more than the diagnosis itself.
What does a sciatica flare-up feel like, and why does it happen?
A flare-up is a sudden increase in pain. It often starts after a trigger.
Sudden triggers
Common triggers include:
- Lifting something heavy
- Twisting the spine
- Sitting for long periods
These movements increase pressure on the nerve.
Inflammation spike
After the trigger, the body reacts. The area around the nerve becomes irritated. This increases sensitivity and makes the pain feel stronger.
Why does pain increase over the day
Pain often builds as the day goes on.
This happens because:
- You sit more
- The spine takes more load
- The nerve stays irritated longer
Why mornings sometimes feel better
After lying down overnight, pressure on the spine is lower. This can reduce irritation for a short time. As the day starts and movement increases, symptoms return.
How do you make sciatic nerve pain stop hurting? (Real decision guide)
Relief depends on timing and the right type of movement.
First 48 hours (inflammation phase)
Focus on reducing irritation.
- Use ice for short periods
- Avoid long sitting
- Do not stay in bed all day
After 2–3 days (movement phase)
Start controlled movement.
- Short walks
- Light activity
- Avoid heavy lifting
Rest vs movement (what research says)
Too much rest slows recovery.
Research in the Journal of Orthopaedic & Sports Physical Therapy (JOSPT) shows that staying active leads to better outcomes than bed rest.
Sitting, sleeping, posture adjustments
- Sit for short periods only
- Keep your back supported
- Avoid slouching
- Sleep in a position that reduces strain on the lower back
DO vs DON’T
Do:
- Move regularly
- Change positions often
- Use controlled exercises
Don’t:
- Sit for long hours
- Stay in bed for days
- Do random stretches without understanding your pain
3 home exercises that may reduce nerve pressure (with logic)
Exercises help when they match the cause.
Exercise 1 — McKenzie extension
This exercise involves gently arching your back. It helps push disc material away from the nerve. This can reduce pressure in disc-related cases.
It may also move pain from the leg back toward the back. This is a good sign.
Exercise 2 — Piriformis stretch
This stretch targets a muscle in the butt area. It helps when the muscle is pressing on the nerve. It is not useful for disc-related cases.
Exercise 3 — Nerve glide (flossing)
This involves gentle movement of the leg to improve nerve mobility. It helps the nerve move more freely and reduces stiffness.
Studies in JOSPT and the Journal of Manual Therapy support its use in some cases.
When not to do these
- If pain becomes sharper or spreads further down the leg
- If you feel increased weakness
- If symptoms worsen quickly
Stop and reassess.
What is centralization, and why does it tell you if you’re improving
Centralization means pain moves closer to the back. Peripheralization means pain moves down the leg.
What it means
- Pain moving up the leg → improvement
- Pain moving down the leg → worsening
Example:
- If pain shifts from the foot to the thigh, that is a good sign.
- If it moves from the back to the foot, that is not.
This concept is widely used in physical therapy.
How long does sciatic nerve pain take to heal?
Recovery happens in stages.
- Phase 1 — Inflammation (0–7 days): Pain is high. The area is sensitive.
- Phase 2 — Stabilization (1–4 weeks): Pain becomes more stable. Movement improves.
- Phase 3 — Recovery (4–12 weeks): The nerve becomes less sensitive. Function improves.
Studies from the BMJ and the Spine Journal show that many cases improve over time without surgery.
Why nerves heal more slowly
Nerves recover more slowly than muscles. That is why symptoms can last longer even after the main issue improves.
When should you worry about sciatic nerve pain?
Most cases improve. Some need urgent care.
Red flags
- Loss of bladder or bowel control
- Numbness in inner thighs
- Severe weakness in the leg
These may indicate a serious condition.
Progressive weakness
If the strength in your leg keeps getting worse, seek medical care.
When to seek imaging
- Pain lasting more than a few weeks
- Symptoms getting worse
- No improvement with basic care
The Mayo Clinic recommends evaluation in these cases.
Why most people make sciatic pain worse without realizing it
Small mistakes can delay recovery.
- Staying in bed too long
- Following random online exercises
- Sitting for long hours without breaks
- Returning to heavy activity too early
These increase pressure on the nerve and slow healing.
FAQ
How do you know if it’s your sciatic nerve?
Pain that travels down one leg with tingling or numbness usually points to nerve involvement.
What does a sciatica flare-up feel like?
It feels like a sudden increase in sharp or burning pain, often after movement or long sitting.
What is mistaken for sciatica pain?
Muscle strain, piriformis syndrome, and spinal stenosis are common conditions that feel similar.
How do I make my sciatic nerve stop hurting?
Reduce pressure on the nerve with the right movement, avoid long sitting, and follow a structured approach.
Can sciatica go away on its own?
Yes, many cases improve over weeks, but proper management speeds recovery.

Recent Posts